Newsletter Signup - Under Article / In Page
"*" indicates required fields
Taking advantage of the ability of viruses to manipulate life is opening new doors for the biotech industry. Once only seen as our enemies, viruses are fast becoming some of our most valuable allies.
Viruses may not have the best public image, but to biotechnologists, there’s a lot to admire about them. These tiny molecular machines have unparalleled abilities, honed over billions of years of evolution, to infiltrate and exploit living beings — including ourselves.
Domesticating viruses has been an ongoing scientific endeavor for decades. Their talents as cellular hijackers make them extremely valuable as tools for a wide variety of biotech applications, from delivering gene therapies to killing superbugs.
Bacteria-eating viruses
The threat of antimicrobial resistance was labeled “as big a danger to humanity as climate change or warfare” by the UK’s Health Secretary at the World Economic Forum last year. Indeed, antibiotic-resistant infections are on track to kill 10 million people a year by 2050.
As the number of effective antibiotics in our arsenal continues to dwindle, there is an increasing interest in tackling superbugs using bacteriophage viruses, which are natural predators of bacteria. These viruses have been killing bacteria for billions of years, and they’ve become very, very good at it.
Bacteriophages, or phages, latch on to their target and hijack its internal machinery to produce more viruses, which then burst out from within the bacterium, destroying it. Conveniently, these viruses are unable to infect human cells, so they are completely harmless to us when used as a therapy against bacterial infections.
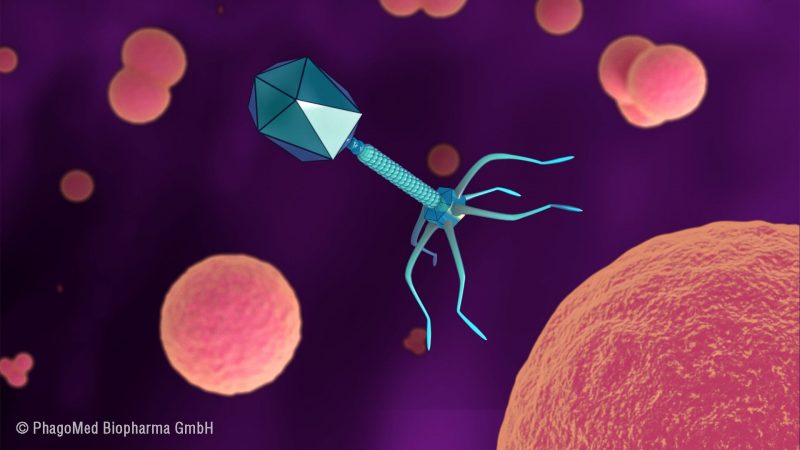
Vienna-based biotech company PhagoMed is pioneering the development of such phage therapy treatments for bacterial infections, with several candidates currently at the preclinical stage.
“Phages are able to kill bacteria irrespective of antibiotic resistance. They have a unique mode of action that can become a much-needed complement to the existing — and increasingly failing — antibiotics therapy,” said Lorenzo Corsini, joint CEO and co-founder of PhagoMed.
Phages also have the added benefit of being extremely precise in which bacterial strains they target. This prevents them from killing beneficial bacteria, which is a common problem with conventional antibiotics.
Of course, there’s still the question of whether bacteria could, in time, evolve resistance to phages as they have to antibiotics. “Eventually, it is possible that individual phages in a [treatment] will have to be replaced,” Corsini told me. “The good news is that by becoming resistant to one phage, bacteria often become susceptible to another phage, so that there is a virtually infinite supply. Phages and bacteria have co-evolved for billions of years, and neither has managed to ‘win’ this evolutionary race.”
Tumor-targeting viruses
Viruses are naturally adept at seeking out and infecting specific cells, making them ideal for targeting tumors with a high level of accuracy while leaving healthy cells undisturbed. Viruses that selectively identify and destroy tumor cells are known as oncolytic viruses.
To date, Amgen’s Imlygic is the only approved cancer therapy based on an oncolytic virus. It consists of a herpes virus that is genetically engineered for treating melanoma. There are many more at various stages of preclinical and clinical development, and there’s been a wave of investment in this area of research from big pharma over the last few years.
In Germany, the firm Oryx Translational Medicine is working to develop the smallest of all oncolytic viruses based on a virus that infects rats in the wild. The virus can selectively kill tumor cells from a wide variety of cancers including glioblastoma and pancreatic cancer, and owing to its small size it is able to pass the blood-brain barrier that protects the brain.
“There was initial skepticism about oncolytic viruses in biotech and pharma,” Bernard Huber, CEO of Oryx told me. “The main challenge for the use of oncolytic viruses is their pathogenicity to humans. Unlike most other oncolytic viruses currently under investigation, ours is not pathogenic to humans and does not affect normal cells or tissues.”
Not only does the virus directly infect and kill cancer cells, but it also profoundly alters the tumor microenvironment, making the tumor more visible to the immune system and increasing its vulnerability to immuno-oncology therapies.
“[Our candidate] has demonstrated an excellent safety profile both as monotherapy and as combination therapy with antibody-based therapeutics, checkpoint inhibitors, or chemotherapy,” Huber explained.
The company has successfully completed two phase I/IIa clinical trials in recurrent glioblastoma and metastatic pancreatic cancer, and is now getting ready to launch a pivotal trial that will support an application for marketing authorization.
Delivering genetic material
Perhaps the most fundamental characteristic of viruses is their inability to self-replicate unless they infect a living cell. To reproduce, they must inject their genetic material into their target and commandeer the cell’s machinery. This ability forms the basis of viral vectors.
Viral vectors are essentially modified viruses that have had the pathogenic components removed from their genome while retaining their gene delivery skills. This makes them incredibly versatile tools for developing technologies that rely on introducing genetic material into human cells, such as gene therapy.
“Viruses have gone through eons of natural selection to make them the most advanced gene delivery tool imaginable, for any and all kinds of tissue and cell types,” said Christian Thirion, founder and CTO of Sirion Biotech, a German company developing viral vectors.
A recent example of a gene therapy reliant on viral vectors is Luxturna, approved in the EU in 2018. Luxturna is designed to treat patients suffering from progressive vision loss due to a specific genetic mutation. The gene therapy uses a viral vector to deliver a functional copy of the mutated gene into retinal cells, restoring the patient’s vision.
There are several types of viral vectors derived from different classes of viruses, including lentiviral vectors based on the HIV virus, adenoviral vectors from common cold viruses, and adeno-associated viral vectors (AAVs) — the ones used in Luxturna.

“AAVs are the new superstars in the gene therapy sector,” Thirion told me. “Wild-type AAVs don’t elicit disease in humans and result in long-term gene expression for up to 10 years. AAVs can be engineered and targeted towards specific cell or tissue types. All these features make them ideal tools for modern gene therapy applications, and the rise in interest in this technology has been steep.”
The surge in demand for viral vectors has triggered an industry-wide shortage over the last year. In response, a growing number of European viral vector developers have recently been scaling up their production, including Sirion Biotech, Oxford Biomedica, Vibalogics, and Cevec.
————
While their sinister reputation may never be fully erased, it’s clear that the more we study viruses, the more impressive they become and the more possibilities they offer us. Far from only being bringers of death and disease, viruses are rapidly establishing themselves as crucial enablers of powerful new treatments that would have been impossible without their help.
Cover illustration by Elena Resko. Images via PhagoMed Biopharma, Sirion Biotech, and Shutterstock. This article was originally published in May 2019 and has been since updated to reflect new developments.






