Best in Biotech 23 Aug 2023
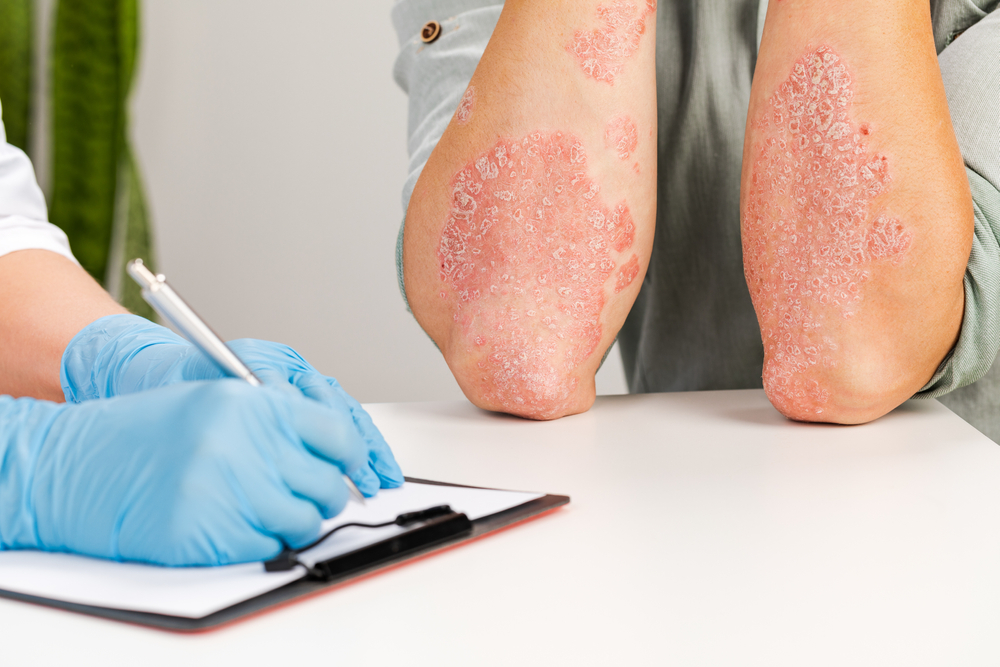
Latest advancements in psoriasis research over the past year
Psoriasis, an autoimmune condition that causes flaky patches of skin to form scales, occurs when the body’s immune system attacks its own healthy skin cells. And because people with psoriasis have an increased production of skin cells, these cells – which are normally renewed every three to four weeks – regenerate in under a week. […]