Scientists have started generating artificial glands using cells derived from urine, which will allow the study of adrenal disorders that affect growth, development, and metabolism.
Researchers at Queen Mary University of London have used cells in urine to begin generating an artificial adrenal gland that could be used to treat adrenal gland disorders. The study, published in Cell Reports, found that steroid-producing cells could be produced by reprogramming cells from the skin, blood, and urine of healthy donors or adrenal disorder patients. These cells were used to model adrenal diseases in a dish and test new personalized treatments and were implanted into mice to check their function.
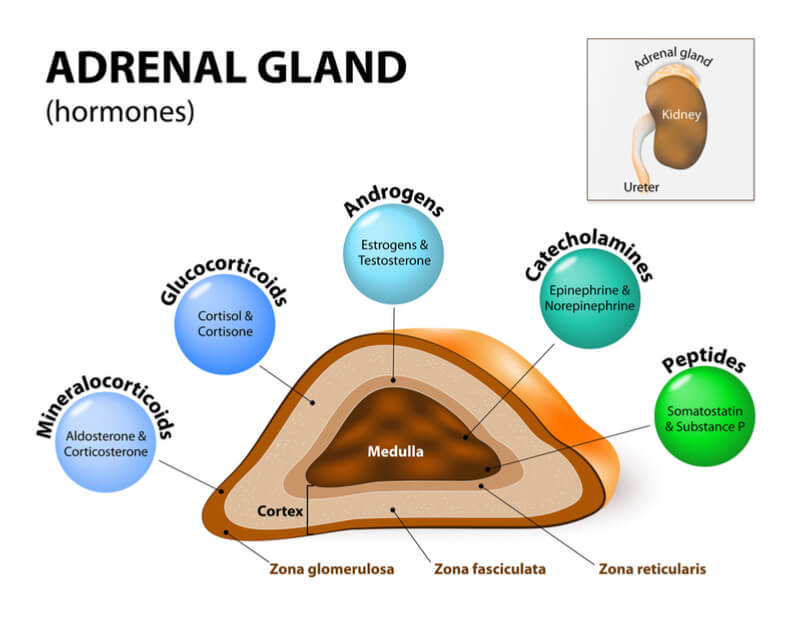
The adrenal glands are found on top of the kidneys and produce a number of hormones, including adrenaline, and the steroids aldosterone and cortisol. Adrenal disorders are caused by genetic mutations, tumors, infections, or problems with other glands, causing the glands to produce too little or too much of a hormone. Addison’s disease is a deadly autoimmune disease caused by a lack of cortisol, leading to symptoms like weight loss, muscle weakness, and low blood pressure.
The research group was able to reprogram cells from the skin, blood, and urine by forcing the expression of a transcription factor. This triggered the activation of two pathways, causing the newly formed human inducible steroidogenic cells (hiSCs) to begin expressing the enzymes required to produce steroids in response to certain stimuli.
Glands produced from the cells of adrenal disorder patients kept their characteristics, meaning they would make effective disease models for the testing of personalized treatments. A gene could also be introduced into these cells to return their steroid profile back to normal, similar to that of glands produced from healthy donors.
Leonardo Guasti, one of the study’s lead authors, commented on the potential of this technology: “It will facilitate the next generation of cell-based treatments for adrenal insufficiency, the modeling of adrenal-specific diseases, and the testing of personalized interventions.”
Looking at the wider applications of the study’s findings, Guasti continued: “It is a first step in generating an artificial adrenal gland which would benefit all patients with adrenal insufficiency. Regenerative medicine for adrenal disorders has been neglected compared to efforts to generate functional endocrine pancreas to cure type-I diabetes. This study closes the gap.”
At the moment, hormone-replacement therapy is the most common treatment for adrenal disorders like Addison’s. However, with this study opening the door to approaches using regenerative medicine techniques, there is potential for the replacement of dysfunctional glands, removing the need for the life-long administration of hormones.
Images – Shidlovski, Designua / shutterstock.com





