Newsletter Signup - Under Article / In Page
"*" indicates required fields
Researchers have developed a skin patch that delivers drugs directly into the blood, avoiding the gut which is a breeding ground for antibiotic resistance.
Researchers at Queen’s University Belfast are developing a skin patch to deliver drugs through the skin and directly into the bloodstream via thousands of ‘microneedles’. The technology is being tested as a potential solution to the growing antibiotic resistance crisis, which is now one of the biggest problems facing society.
Antibiotic resistance is already a massive threat to our health, killing around 700,000 people each year, which is expected to total 10 million by 2050. In particular, it is the oral administration of antibiotics contributes to antibiotic resistance, as the drug interacts with bacteria in the gut. The researchers believe that by avoiding the gut, the lifespan of antibiotics could be considerably improved. The patch has further advantages too. It is discrete and easy-to-use, with its tiny needles painlessly penetrating the top layer of skin to deliver a drug.
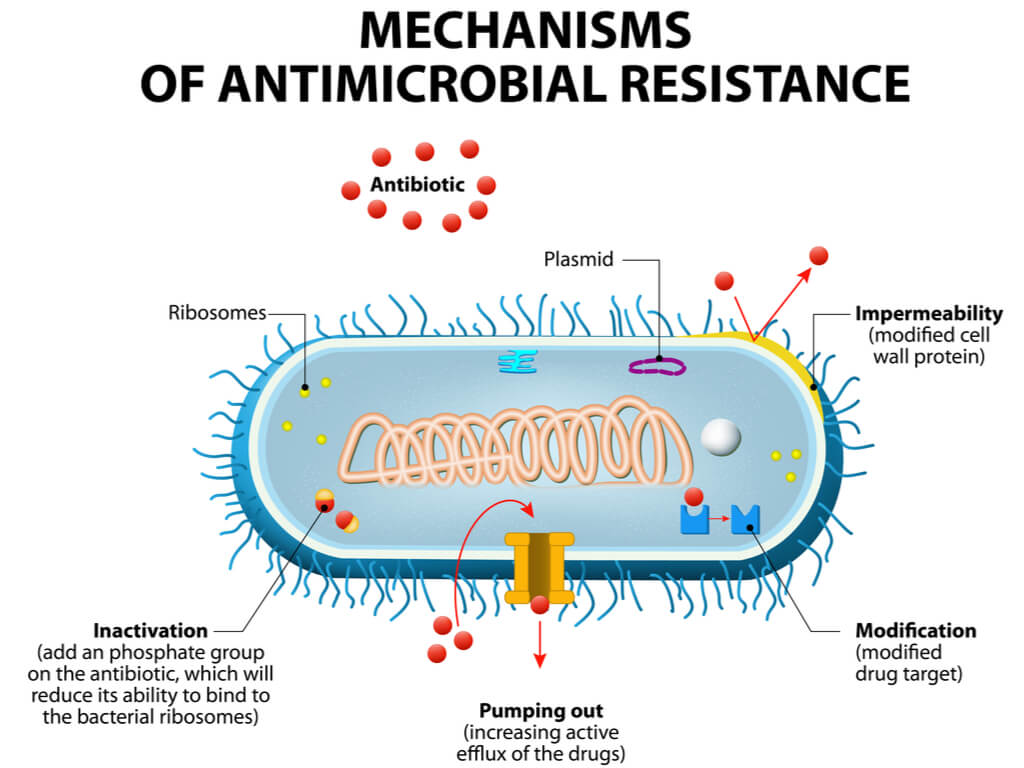
Project leader, Ryan Donnelly, explained why his approach could have such a dramatic effect: “The huge majority of the drugs are taken orally… [meaning] a small quantity of the compound often finds its way into the colon, creating the perfect breeding ground for drug-resistant bacteria.” The intravenous delivery of antibiotics has been shown to significantly reduce resistance but this is impractical: “More than 20% of people are needle-phobic. Admitting patients to hospital every time they need an antibiotic would quickly bankrupt healthcare providers,” he continued.
Patches delivering a placebo have been tested successfully on ten volunteers, and the next step is to see whether the correct dose of antibiotics can be delivered, before comparing it with drugs in capsules.
Donnelly believes that “there probably isn’t a bigger health challenge” than antibiotic resistance, which explains the influx of biotechs into the field. Some big names have switched their attention to the area like Immunocore, which received €33M from the Bill & Melinda Gates Foundation to target its TCR technology at tuberculosis. Da Volterra got €20M from the EU to speed up the development of its medical device that prevents Clostridium difficile infections. Meanwhile, back in the lab, British researchers are harnessing the power of bacterial weapons.
This new approach uses the knowledge that we have accumulated about how and where antibiotic resistance tends to develop and uses it to try and put a stop to it. The development of new antibiotics is a long and expensive process – as with all drugs – but their limited lifespan has put off companies and investors. Technology that prevents the rapid generation of resistance could be just what is needed to encourage more money and expertise back into the field.
Images – Kateryna Kon / shutterstock.com; Designua / shutterstock.com