Researchers from Tel Aviv University (Israel) have managed to engineer a Nanotech ‘heart patch’ which could enable remote monitoring and regulation of a patient’s heart – bionic!
 MedTech continues to blur the boundary between man and machine. A new project combines organic, living tissue and a complex nanoelectronic system to create a bionic heart patch that could help patients recuperate from heart attacks.
MedTech continues to blur the boundary between man and machine. A new project combines organic, living tissue and a complex nanoelectronic system to create a bionic heart patch that could help patients recuperate from heart attacks.
This new technology builds on previous research in tissue engineering for cardiac tissue, which aims to provide an alternative to people who have suffered a heart attack and developed heart failure. Currently, the treatment options are either a heart transplant (not a option for all patients, due to organ shortage) or left ventricular assist devices (VADs) – also not widely available.
Cardiac tissue engineering aims to solve this problem. It combines biomaterials, cells and growth factors, that could replace the heart muscle that was scarred after the infarction – and can no longer contract. This engineered ‘patch’ is implanted in the affected area of the heart.
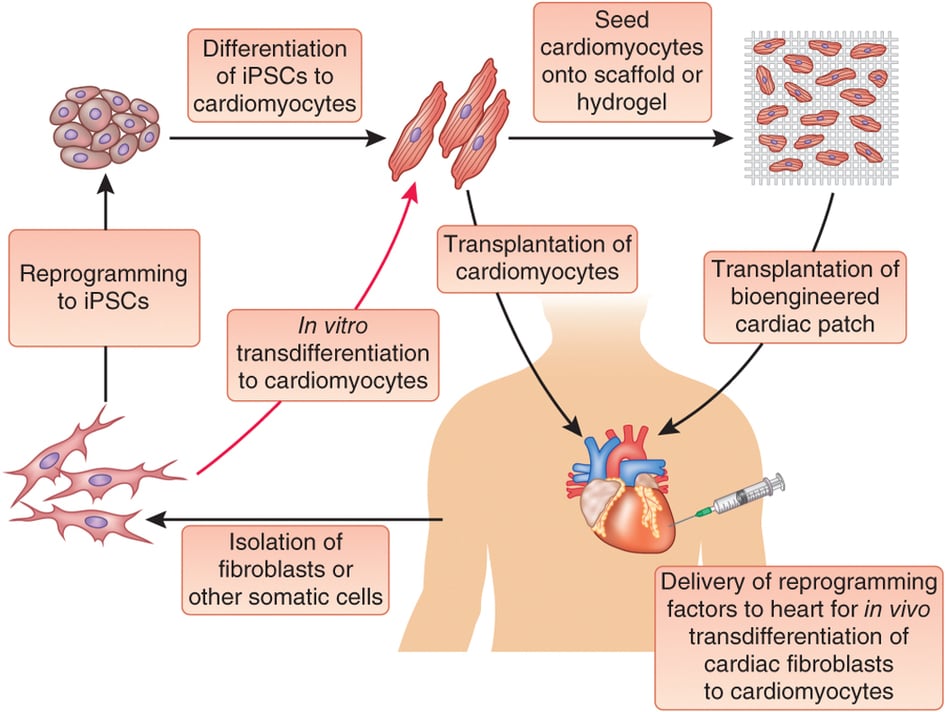
This new heart patch, hailing from Tel Aviv University (TAU), is similarly capable of contracting and expanding like normal heart tissue, but it has a key advantage. By integrating nanoelectronics, the patch can be regulated (or regulate itself) like a machine.
This feature opens new doors for monitoring how the engineered tissue is performing, that can now be evaluated remotely by a physician.
In the future, it could also mean much quicker intervention. If the patch senses inflammation, it would be able release an anti-inflammatory drug. If it senses a lack of oxygen, it will release factors to recruit blood-vessel-forming cells to the affected area…
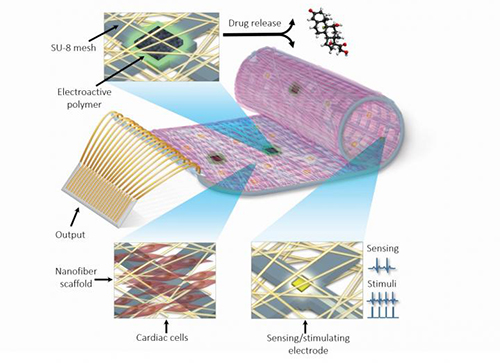
This work was published in the renowned scientific journal Nature Materials and was based off an idea from Tal Dvir and Ron Feiner (at TAU). Making the patch in reality required the collaboration of three different departments: Biotechnology, Materials Science and Engineering, and Nanoscience and Nanotechnology.
This is an amazing breakthrough in combining organic tissue and electronics. But it is, as its inventors note, still a long way from being an approved medical device. The technology needs further development, and to go through the journey of market access (like Carmat‘s artificial hearts are doing now).
The team is also trying to translate this proof of concept to other types of tissue, such as the brain and spinal cord – which could potential to treat several neurological conditions.
Cyborgs and bionics are slowly leaving the realm of over-the-top science fiction and entering practical application in real-life medicine problems – and remain fascinating.