A little biosensor can analyze if there are antibiotics in your blood in 10 minutes. Developed by researchers from the University of Freiburg, the system could be used to develop a personalized course of antibiotics, but also to test food and water. The objective? Slow down the rise of multi-resistant bacteria.
The World Antibiotic Awareness Week is wrapping up, with key health-related institutions like WHO, CDC and the EU launching campaigns to call attention to the threat of antibiotic-resistant ‘superbugs’. Indeed, the recent UK report on the topic, the Review on Antimicrobial Resistance, estimates that by 2050 antimicrobial multi-resistance will be responsible for 10 million deaths, surpassing cancer as a leading cause of mortality.

Almost ready to join the fight against superbugs is an electrochemical biosensor platform, developed at the University of Freiburg, Germany. This device was able to test the presence of two common antibiotics, tetracycline and streptogramin, in small samples of human blood. The success of this proof-of-concept study is now published in the journal Analytical Chemistry.
The system is inspired by the biological mechanism of antibiotic resistance itself. It repurposed a sensor protein that enables resistant bacteria to recognize antibiotics and activate their defense mechanisms. To exploit the protein’s function in a biosensor device, the research team turned to microfluidics, a field that has a lot of interest in novel devices and biohacking. Microfluidic devices also have attracted significant investment, from €1M startups to a huge €455M drug delivery deal.
The potential of the biosensor goes beyond these initial results with two antibiotics. The microfluidic chips can measure up to 8 different substances at the same time, have a shelf life of 3 months. The analysis itself that takes only 10 minutes.
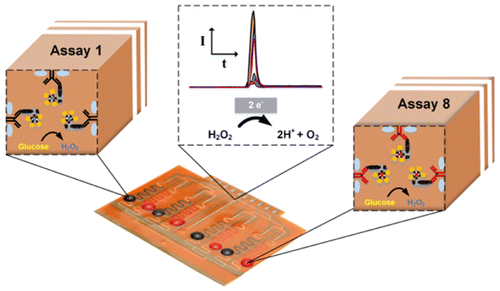
The most immediate application of these microfluidic chips is in the clinic, as a point-of-care test. The next step of research is to develop a method to determine how quickly the human body breaks down antibiotics, thus enabling the dosage to be adjusted to each patient. This personalized take on antibiotics not only improves the treatment, but also gives pathogens less ‘chances’ to become resistant. The devices could also be used in environmental and food safety testing, to analyse potential contaminations of food and water – a result of intensive use of antibiotics in agriculture.
Therefore, this chip could provide a simple way to monitor the presence of antibiotics in ourselves and the environment, tackling the root causes of the antibiotic resistance threat. It would certainly be a worthy addition to this Biotech fight, that goes from better diagnostics to novel antibiotics, some directly targeting resistance mechanisms, and more exotic solutions like bacteriophages and CRISPR.
Images: WHO, Kling et al. (2016) Multianalyte Antibiotic Detection on an Electrochemical Microfluidic Platform. Analytical Chemistry (doi: 10.1021/acs.analchem.6b02294)