A European academic research collaboration has found a new potential weapon against antibiotic-resistant tuberculosis: its own toxins.
Many types of bacteria, such as the pathogen responsible for the deadly lung disease tuberculosis, Mycobacterium tuberculosis, use toxins to stay alive. For example, these toxins can be useful when the bacteria are starved or infected by viruses, and need to grow less, or commit suicide for the good of the colony. The dangerous effects of the toxins are tightly controlled by the bacterium, which produces antitoxins that can block them.
A team of researchers from centers in France, Germany and the UK targeted one of these toxin-antitoxin systems in M. tuberculosis. As the toxin in this system is basically a suicide molecule for the pathogen, they investigated its potential for treating tuberculosis infections, many of which are becoming increasingly resistant to traditional antibiotics.
“This is a new approach, as all currently used approaches target essential enzymes in the bacillus,” Olivier Neyrolles, the leading researcher from the Institute of Pharmacology and Structural Biology, France, told me. “Here, we don’t want to target an essential enzyme but to release a toxic natural product of the bacterium.”
After characterizing the system, the researchers infected mice with an engineered strain of M. tuberculosis that inducibly expresses the toxin without its antitoxin. They found that inducing the expression of this toxin improved the survival rate of the tuberculosis-infected mice by 40% compared with controls.
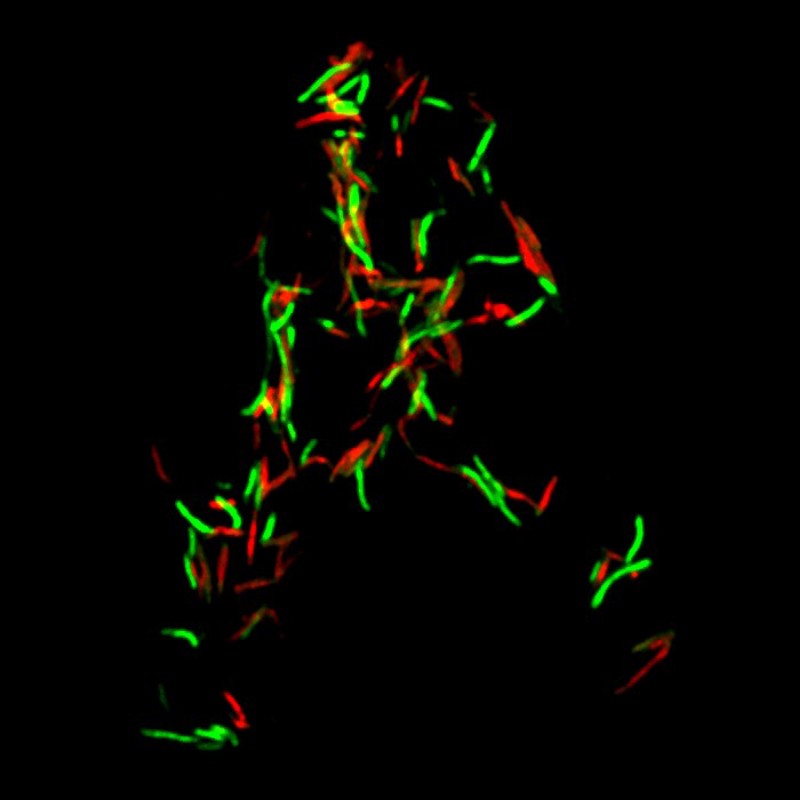
Published in Molecular Cell, these promising results make this toxin-antitoxin system a potential avenue for future tuberculosis treatments. The researchers believe that this could also form the basis for treating infections of other types of drug-resistant bacteria.
“New antibiotics that work in completely different ways are essential for treating multi-drug resistant infections,” Luiz Pedro Carvalho, one of the collaborating researchers at the Francis Crick Institute, UK, told me. “Using a mechanism intrinsic to the bug, such as a toxin-antitoxin pair, has never been used before, and in theory might lead to fewer mutations and therefore less resistance.”
The researchers now plan to look for therapeutic molecules that can disrupt the suicide systems in bacteria like M. tuberculosis, causing the toxins to get out of control and kill the cells.
The war against drug-resistant bacteria is raging in Europe, with many efforts to prevent, circumvent or break antibiotic resistance. Tuberculosis is also the target of a collaboration between the UK cancer immunotherapy biotech Immunocore and the Bill and Melinda Gates Foundation. A drug from the University of Manchester, UK, also showed promise for activating the immune system to fight tuberculosis in mice last September.
Images from Shutterstock and The French National Centre for Scientific Research (CNRS)