Newsletter Signup - Under Article / In Page
"*" indicates required fields
A new ‘organ-on-a-chip’ device for the blood-retina barrier could speed up the development of treatments for eye diseases like retinitis pigmentosa.
Researchers from Microelectronics Institute of Barcelona, Vall d’Hebron Research Institute, and Universitat Autònoma de Barcelona have developed a microfluidic chip that mimics the human blood-retinal barrier in the eye. The study, published in Lab on a Chip, sets out how the design of the device replicates the structure of the retina.
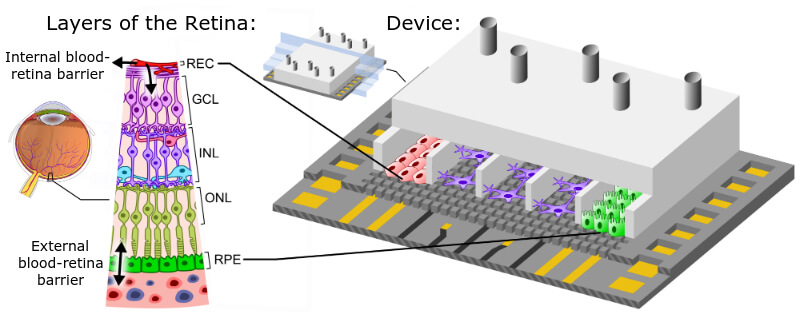
The device is composed of several parallel compartments that recreate the layered structure of the retina. In each compartment, a specific cell type is grown to replicate the different layers as closely as possible. For example, endothelial cells represent capillaries, neurons take the place of the neuroretina, and retinal pigmented epithelial cells make up the device’s external blood-retinal barrier.
The compartments are interconnected by microgrooves, allowing the exchange of signal molecules between cells, reproducing the sort of cellular communication seen in the body. Additionally, the device exposes endothelial cells to the mechanical conditions that they experience from the bloodstream. Rosa Villa, a scientist at the Spanish Council for Scientific Research, explained the importance of recreating these effects: “In cell cultures, where this condition is not reproduced, we could say the cells are ‘sleepy’ and do not react as they would do in real conditions”.
This work builds on a previous device developed by Villa’s team that emulates the blood-brain barrier. These devices will hopefully help to reduce animal testing and accelerate research and clinical trials for eye diseases like diabetic retinopathy.
Loss of vision is an area of great interest for biotechs and patients alike. Glaucoma and retinitis pigmentosa – a genetic disease characterized by a loss of photoreceptor cells in the retina – are common causes of blindness. Gene therapy has been used to correct the mutations causing retinitis pigmentosa by a number of biotechs like Horama, which targets mutations in the PDE6β gene, and NightstaRx for mutations in the RPGR gene. Meanwhile, GenSight has combined gene therapy with a wearable device to treat retinitis pigmentosa cases caused by 1 of up to 100 different mutations.
If I was suffering from a disease that caused me to lose my sight, I would definitely be frantically searching for any help that I could. However, the future looks bright, with new technology like this being developed, and biotechs developing therapeutic approaches that are progressing well through the clinic.
Images – AnnaVel / shutterstock.com; Microelectronics Institute of Barcelona
Are you interested in eye disease R&D?







