Researchers at the University of Cambridge believe that they have found the region of the brain that is responsible for pain relief, which should help future drug development efforts.
Scientists at the University of Cambridge have identified the area of the brain that is responsible for pain relief, which could boost the development of alternative forms of analgesia. A study, published in eLIFE, found that the pregenual cingulate cortex, found in the prefrontal cortex, is important in controlling pain, meaning biotech and pharma companies have something new to work with when developing new pain relief drugs.
Pain plays an important role in our survival, telling us to stop if we are hurt. For this reason, Ben Seymour of the University of Cambridge’s Department of Engineering describes pain as “healthy.” However, this may not be so reassuring to patients suffering from chronic pain due to conditions like osteoarthritis. These individuals have to make do with opioids and non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen, which are associated with addiction and cardiovascular events, respectively.
Seymour’s group carried out two experiments to find out the control of pain by the brain. First, they attached a metal probe to the arm of healthy volunteers and heated it until it started to cause pain. The volunteers’ brain activity was monitored so that the researchers could find out what a pain signal looks like. This allowed the researchers to spot that the signal was taking place in the pregenual cingulate cortex, a region in the brain’s prefrontal cortex, during a second experiment.
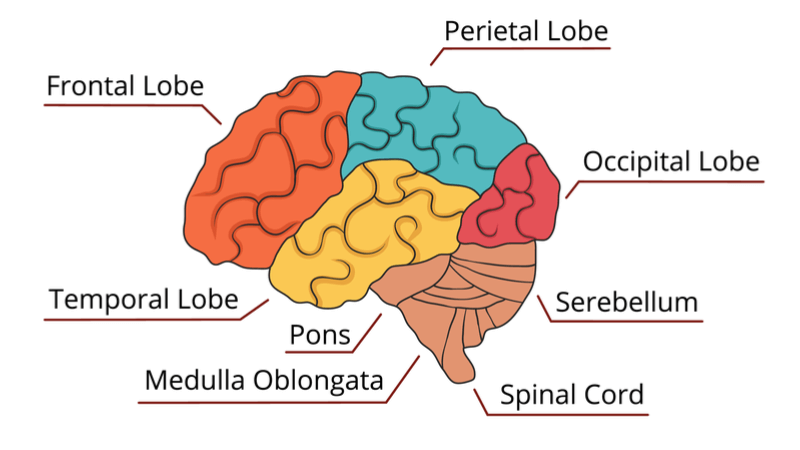
Seymour believes that “these results build a picture of why and how the brain decides to turn off pain in certain circumstances and identify the pregenual cingulate cortex as a critical ‘decision center’ controlling pain in the brain,” which puts it forward as a target for future research efforts.
Current efforts to develop new pain relief medicines focus on modulating nerve growth factor (NGF) to keep pain signals under control. Pfizer and Eli Lilly’s monoclonal antibody, tanezumab, inhibits NGF to control pain effectively. However, when it was tested for the treatment of osteoarthritis, it sped up joint deterioration. The British biotech, Levicept, was set up to overcome this with its fusion peptide, LEVI-04, which is undergoing a Phase I trial.
In a recent interview with Levicept’s CEO, Simon Westbrook, I found out that: “There hasn’t been a new pain drug on the market for almost 30, 40 years… the most recent one was probably Betapam, which is really old.” Despite this clear market opportunity, and the pain relief market set to be worth $83B (€67B) by 2024, there is very little investment and interest in the field.
A market analysis by BIO found that the very low clinical success rate of just 2% – far lower than the 10% average – could be enough to discourage pharma and biotech companies from entering the field. This must be in part responsible for the low investment in the pain relief field, which receives 17 times less investment than oncology.
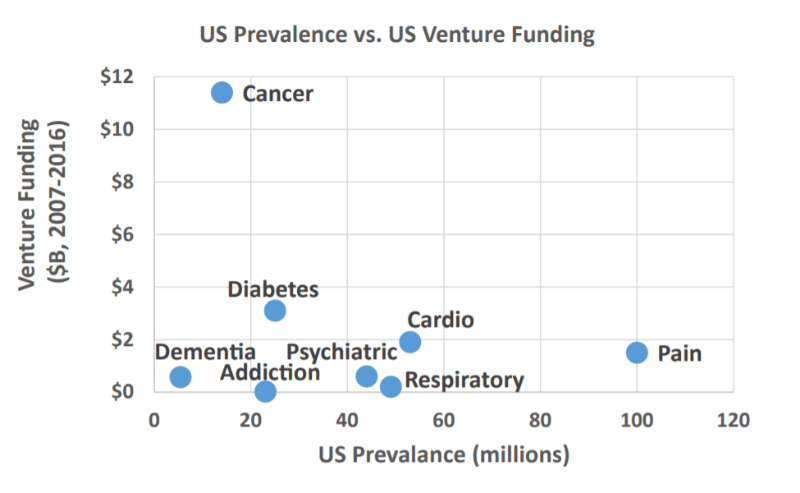
These numbers highlight the problem that patients suffering from chronic pain face – what they have available to them isn’t good enough and there isn’t enough being done to change that. However, the research carried out at the University of Cambridge could be just what is needed to attract more attention and investment into the pain relief field.
Images – kubicka / shutterstock.com; Pretty Vectors / shutterstock.com; Oxy_gen / shutterstock.com; Endpoints